Deep Brain Stimulation (DBS) Surgery Cost in India
Deep brain stimulation (DBS) Surgery is a life-changing neurosurgical procedure that has transformed the lives of countless individuals struggling with debilitating neurological conditions.
For those with Parkinson’s disease, DBS Surgery can significantly improve motor control, allowing them to regain independence and participate in activities they once thought were out of reach.
DBS has also shown promise in treating epilepsy, obsessive-compulsive disorder (OCD), and Tourette’s syndrome.
The impact of DBS extends beyond symptom management and includes:-
- It can profoundly enhance patients’ overall well-being.
- Individuals report improved mood, increased energy levels, and a renewed sense of hope.
- Regaining control over their bodies and minds empowers patients to engage more fully in life’s activities and pursue their aspirations.
After DBS surgery, a patient can be confident again, as there is no more social stigma, and go back to work to become financially independent. also, the economic benefits of not having to pay for medication are what make DBS one of the most effective treatment.
DBS Surgery opens a new chapter of hope and possibility.

Deep Brain Stimulation (DBS) Surgery Cost in India ranges between 17,500 USD using non-rechargeable – 24000 USD with rechargeable.
It is important to note that this is an estimated cost and the actual cost may vary. It is best to consult with a neurosurgeon or a healthcare provider for an accurate quote and to understand the various costs associated with the procedure.
The hospital stay is 3 days and 7 days outside of the hospital.
Tests demanded until DBA are MRI, CT scan, tests for memory, mood, and thinking.
That is FDA-approved treatment using a success rate of over 95%.
[Verified by:- Dr Himanshu Champaneri, Director , MBBS, MS, FMAS, DNB, Fellowship 14 Years of Experience Gurgaon, India. (Updated On 22/july/2024 ]
What is Deep Brain Stimulation?
Deep Brain Stimulation (DBS) is a neurosurgical technique that involves the implantation of electrodes into specific areas of the brain. These electrodes are connected to a battery-powered generator, which is implanted under the skin near the collarbone. The generator produces electrical impulses that are delivered to the brain through the electrodes, which can regulate brain activity and help to improve symptoms in certain conditions such as Parkinson’s disease, essential tremor, dystonia, obsessive-compulsive disorder (OCD), and depression.
DBS is typically used as a treatment option for patients who have not responded well to other forms of treatment, such as medications or physical therapy. It works by stimulating the specific areas of the brain that are involved in controlling movement, mood, or other symptoms. The electrical impulses help to regulate the activity of the brain cells, which can improve symptoms and improve quality of life.
DBS is considered a safe and effective treatment option for many patients, but like any surgery, it carries risks such as infection, bleeding, and damage to the surrounding brain tissue. It is important to discuss the risks and benefits of DBS with a healthcare provider before deciding if it is the right treatment option for you.
What is deep brain stimulation?
It is typically used for conditions like Parkinson’s disease, dystonia, tremors, etc that are resistant to other forms of treatment. The procedure involves two parts:
- Placement of electrodes at the targeted brain area(s):- The surgeon needs to locate the areas of the brain which need to be targeted. This is done through an MRI/CT scan or electrode recording technique. Electrodes are placed in the target area, with the loose ends placed under the skin of the head. This procedure is done under general anesthesia.
- Placement of pacemaker in the chest:- Under general anesthesia, a pacemaker is placed just below the collarbone under the skin of the chest. It is connected to the electrodes using extension wires.
Signals are generated from the pacemakers and sent to the brain, which block the impulses that cause tremors in various parts of the body.
Know more about Deep Brain Stimulation
Risk of Deep Brain Stimulation (DBS) Surgery
Deep brain stimulation involves creating small holes in the skull to implant the electrodes, and surgery to implant the device that contains the batteries under the skin in the chest. Complications of surgery may include:
- Temporary tingling in the face or limbs
- Temporary pain/swelling at implantation site
- Allergic reaction to the implant
- Slight paralysis
- Speech or vision problems
- Jolting or shocking sensation
- Loss of balance
- Dizziness
- Reduced coordination
- Concentration difficulties.
Deep brain stimulation is hence a cost vs. benefits problem. For many patients with treatment-resistant forms of Parkinson’s disease and other movement disorders, DBS can help them return to a normal life and regain quality of life.
Deep brain stimulation is not a cure, it is a way to manage unmanageable symptoms that interfere with normal functions.
Symptoms Of Deep brain stimulation Surgery
- You may have some soreness in the head, neck and chest.
- You may develop painless puffy swelling around the eyes for a few days after surgery, particularly the eye under the incision(s).
- You may experience a micro-effect after surgery. This means that some of your symptoms may be better for a few days. This will fade away and you can expect to return back to your previous level of functioning.
- If you have Parkinsons’ disease and experience more dyskinesias, you may have to decrease your Parkinson’s disease medications. Unless it is severe, it is usually best to wait as this generally improves with resolution of the micro-effect.
How does DBS Surgery work?
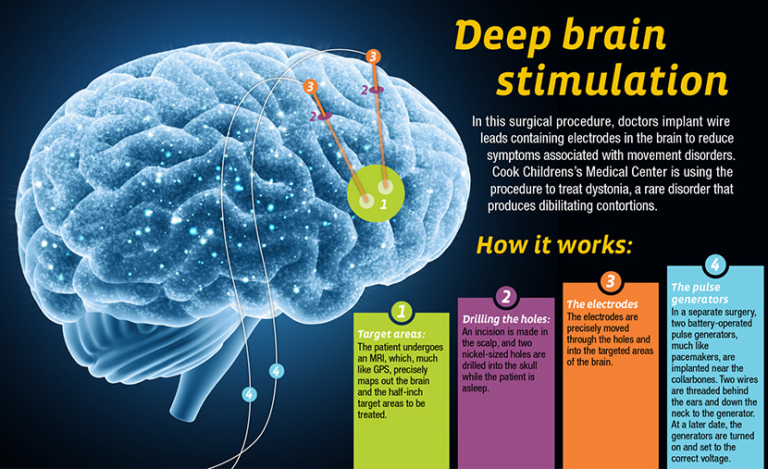
Deep Brain Stimulation (DBS) surgery is a neurosurgical procedure that involves implanting electrodes into specific areas of the brain. The electrodes are connected to a battery-powered generator, which is implanted under the skin near the collarbone. The generator produces electrical impulses that are delivered to the brain through the electrodes, which helps regulate brain activity and improve symptoms in certain conditions such as Parkinson’s disease, essential tremor, and dystonia.
During DBS Procedure
Here is a general overview of the DBS surgery procedure:
Planning and preparation: Before the surgery, the patient undergoes various imaging and diagnostic tests to identify the target location for the electrodes. The patient and the surgeon also discuss the risks and benefits of the procedure and the expected outcomes.
Anesthesia: The patient is given general anesthesia, which puts them to sleep and ensures that they don’t feel any pain during the procedure.
Making a burr hole: The surgeon makes a small hole in the skull, which is known as a burr hole. This hole is used to insert the electrodes into the brain.
Electrode placement: The electrodes are inserted through the burr hole and positioned in the target area of the brain. The electrodes are then connected to the generator.
Closing the incisions: The burr holes are closed and the generator is secured under the skin near the collarbone.
Testing and programming: After the surgery, the generator is programmed to deliver the electrical impulses at specific times and intensities. The patient’s response to the stimulation is monitored and the settings are adjusted as needed to optimize the benefits.
Recovery after DBS Surgery?
The patient is expected to stay in the hospital for 1-2 days after the surgery. Recovery time is quick, though there might be disorientation or itchiness near the stitches initially.
During the recovery time after implanting the electrodes, you may feel better than normal. Brain swelling around the electrode tip causes a lesion effect that lasts a couple days to weeks. This temporary effect is a good predictor of your outcome once the stimulator is implanted and programmed.
About a week later, you will return to the hospital for outpatient surgery to implant the stimulator in the chest/abdomen. This surgery is performed under general anesthesia and takes about an hour. Patients go home the same day.
Results
Deep brain stimulation won’t cure your disease, but it may help lessen your symptoms. If deep brain stimulation works, your symptoms will improve significantly, but they usually don’t go away completely. In some cases, medications may still be needed for certain conditions.
Deep brain stimulation isn’t successful for everyone. There are a number of variables involved in the success of deep brain stimulation Surgery. It’s important to talk with your doctor before surgery about what type of improvement you can expect for your condition.
Frequently Asked Questions DBS Surgery
Q.How long does deep brain stimulation surgery take?
A. The length of the operation also depends on the technique used by each center, but it often lasts between 3-6 hours from start to finish. As long as the electrodes are accurately placed, without complications, the recovery period usually lasts from between 3 to 5 days.
Q. What is the success rate of deep brain stimulation surgery in India?
A. Studies report that DBS Surgery can reduce off -periods of PD symptoms by 60% (fluctuations in motor symptoms due to poor response to medicines). By reducing the need for medication, DBS Surgery rapidly decreases medication-induced dyskinesias by 60 to 80% and improves the quality of life in people with advanced PD.

Dr Aditya Gupta
Neurosurgeon, Gurgaon, India Director, 28 years of experience.

Dr. Himanshu Champaneri
Neurosurgeon, Gurgaon, India. Senior Consultant, 14 Years of Experience.

Dr Vikas Gupta
Neurosurgeon, New Delhi, India Director, 36 years of experience.



